What if your period wasn't a monthly surprise, but a forecasted event you could actually prepare for? Most women view midlife cycles as a chaotic descent into the unknown. You're likely tired of ruined plans because of a sudden start or the anxiety of a "flooding" episode at work. You need a clear framework for perimenopause bleeding patterns what to expect. Tracking is history. Anticipation is the future.
By 2030, 2 billion women globally will be postmenopausal. You don't have to navigate this transition blindly. We'll show you how to distinguish between spotting and a light period using the October 2025 European Society of Endocrinology guidelines. You'll learn exactly when a shift in flow is a normal hormonal pivot and when it's time to call your doctor. We're replacing the anxiety of the unknown with the clarity of clinical data. It's time to move from passive endurance to informed control.
Key Takeaways
- Understand the biological shift behind your changing cycle. Irregularity is the new normal during this decade-long transition.
- Identify seven distinct perimenopause bleeding patterns what to expect. Move from confusion to clarity.
- Learn the "Soaked Pad" rule. Know exactly when your symptoms require a doctor's visit.
- Shift your focus from tracking the past to anticipating the future. Use data-driven insights to regain control over your schedule.
Decoding the Chaos: What to Expect from Perimenopause Bleeding Patterns
Perimenopause isn't a medical failure. It's a biological transition. Your ovaries are becoming less sensitive to the hormonal signals they've followed for decades. This decline in sensitivity triggers the erratic perimenopause bleeding patterns what to expect as you navigate a transition that typically spans 4 to 10 years. For many women, irregular is the new normal. It's a physiological shift that demands a new strategy.
Your anxiety over these changes is valid. Hormonal fluctuations are biologically disruptive. They aren't just "in your head." These shifts impact your vascular system, your brain chemistry, and your daily productivity. Understanding the mechanics of perimenopause allows you to stop reacting to your body and start preparing for it. Tracking looks at the past. Anticipation looks at the future.
To better understand how to manage sudden bleeding episodes, watch this helpful video:
The Biological Shift: Estrogen vs. Progesterone
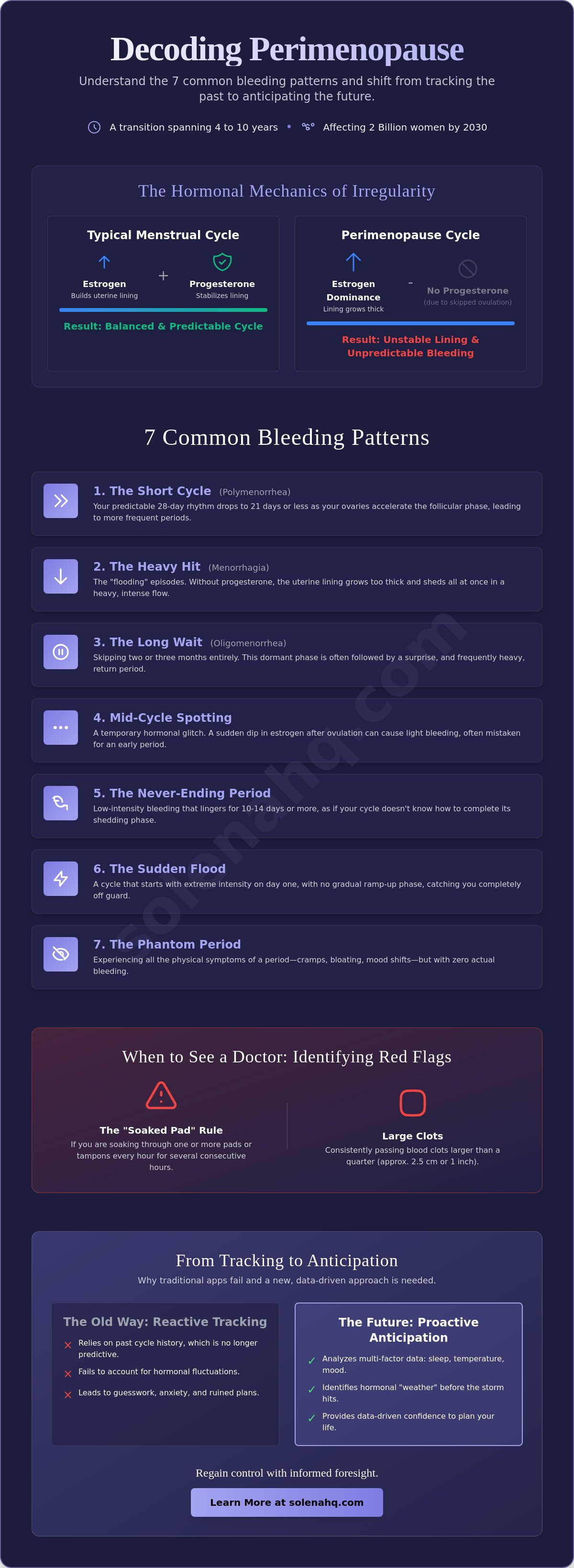
During a typical cycle, estrogen builds the uterine lining and progesterone stabilizes it. In perimenopause, your body often skips ovulation. When this happens, you don't produce the progesterone needed to signal the lining to stop growing. This leads to "estrogen dominance." The result is a lining that becomes thick and unstable, eventually shedding in heavy, unpredictable episodes. Anovulatory cycles are the primary cause of these pattern shifts.
Why Traditional Tracking Apps Fail in 2026
Standard calendar-based algorithms are designed for regularity. They look at your last three months and guess the date of your next period. In perimenopause, your past no longer predicts your future. These apps break because they ignore the physiological "noise" that precedes a bleed. You need a more sophisticated approach.
Modern foresight requires multi-factor data. By monitoring sleep quality, basal temperature, and mood shifts, you can identify the hormonal "weather" before the storm hits. We're shifting the focus from "when will it start" to "how will I feel." This data-driven confidence allows you to schedule your life with precision rather than guesswork. You don't need a history lesson. You need an alert system.
7 Common Bleeding Patterns You May Encounter
Understanding your cycle requires moving beyond the vague label of "irregular." It's about identifying specific biological signatures. Every woman experiences changes in her menstrual flow differently, but patterns usually fall into distinct categories. Here is the breakdown of perimenopause bleeding patterns what to expect as your hormones recalibrate for the next phase of life.
- The Short Cycle (Polymenorrhea): Your predictable 28-day rhythm suddenly drops to 21 days or fewer. This happens because the follicular phase accelerates. Your ovaries are working harder to stimulate an egg, leading to more frequent periods.
- The Heavy Hit (Menorrhagia): This is the "flooding" many fear. Without enough progesterone to stabilize the uterine lining, it grows too thick and sheds all at once. This pattern is a major contributor to the US$150 billion annual global economic cost of menopause related productivity loss.
- The Long Wait (Oligomenorrhea): You might skip two or three months entirely. This isn't menopause yet. It's a dormant phase before a surprise, often heavy, return.
- Mid-cycle Spotting: A sudden estrogen dip after ovulation can cause light bleeding. It's often mistaken for a period, but it's actually a temporary hormonal glitch.
- The Never-Ending Period: Bleeding that lingers for 10 or 14 days at a very low intensity. It feels like your cycle simply doesn't know how to turn off.
- The Sudden Flood: A cycle that starts with extreme intensity on day one with no ramp up phase.
- The Phantom Period: All the physical symptoms of a period with zero actual blood.
The Spectrum of Blood Color and Texture
Color is a data point. Bright red blood indicates active, rapid shedding. It's fresh. It's moving quickly through the cervix. Brown or dark discharge is simply old blood. It has oxidized because the shedding process is slow or stalled. If you notice clots larger than a quarter, your lining is likely shedding in chunks rather than liquid. This is common during heavy hits. It warrants attention if it's constant. Monitoring these shifts helps you prepare your wellness plan with precision.
The 'Phantom' Period
You feel the cramps. Your breasts are tender. The bloating is unmistakable. Yet, nothing happens. This phantom period occurs when your brain signals for a cycle, but your ovaries don't respond with enough estrogen to build a shed-able lining. Your body is trying to cycle. It's a silent hormonal peak. AI identifies these patterns by analyzing your sleep quality and temperature, even when the blood isn't there to confirm it. This is why we focus on perimenopause bleeding patterns what to expect from a holistic data perspective. You aren't imagining the symptoms. Your hormones are simply speaking a different language.
The Hormonal Mechanics of Irregularity
Your body isn't malfunctioning. It's fighting a biological battle. The brain doesn't let the ovaries retire quietly; it fights back by surging Follicle Stimulating Hormone (FSH). Your pituitary gland is essentially shouting at your ovaries to produce an egg. When they finally respond, they often do so with excessive force or not at all. This creates the erratic perimenopause bleeding patterns what to expect during this transition. It's a high-stakes dialogue between your brain and your reproductive system.
Cycle length is primarily dictated by the luteal phase, the time between ovulation and your period. In perimenopause, this phase often shrinks from the standard 14 days to 10 or fewer. This contraction is why your 28-day cycle suddenly becomes a 21-day cycle. It's helpful to use a Perimenopause Symptom Checker to see if your cycle changes align with these specific hormonal shifts. Understanding the "why" removes the panic from the "when."
Stress acts as a biological accelerant during perimenopause and irregular periods. Cortisol and progesterone share the same molecular precursor. When you're stressed, your body prioritizes cortisol production, effectively "stealing" the building blocks needed for progesterone. This creates additional hormonal noise. It turns a manageable shift into a chaotic disruption.
Estrogen Surges and the 'Second Puberty'
Perimenopause is puberty in reverse. It's not a linear decline; it's a series of spiky peaks. In late perimenopause, estrogen levels can surge to heights 30% higher than your baseline in your 20s. These aggressive spikes are the direct cause of sudden breast tenderness and the heavy "flooding" episodes discussed earlier. Your body is navigating an intense biological recalibration. These spikes are temporary, but their impact on your flow is immediate.
Progesterone: The Missing Peace
Progesterone is typically the first hormone to decline significantly. Think of it as the uterine stabilizer. Without it, the lining becomes fragile and prone to breaking down at random intervals. This lack of support leads to "lining instability," resulting in the spotting and unpredictable starts that ruin plans. You can learn more about managing these shifts in our guide on Progesterone for Menopause. When you anticipate the drop, you can prepare for the flow. Control starts with data.
When to See a Doctor: Identifying Red Flags
Chaos has its limits. While fluctuations are part of the transition, certain perimenopause bleeding patterns what to expect cross the line from "normal shift" to "medical priority." You shouldn't have to guess if your flow is dangerous. Clarity comes from clinical benchmarks. These red flags are your signal to stop monitoring and start acting. It's about safety, not just convenience.
The "Soaked Pad" Rule is your primary metric. If you're soaking through one or more pads or tampons every hour for a full afternoon, that's clinical menorrhagia. It's not just a heavy day. It's a risk for anemia. Understanding perimenopause bleeding patterns what to expect means knowing that bleeding lasting longer than 7 days consistently or cycles occurring more frequently than every 21 days require investigation. If you've had 12 months of silence, any amount of blood is an emergency. Post-menopausal bleeding is never "just a late period." It's a critical alert.
Post-Surgical and Specialized Scenarios
Context matters. If you've had a hysterectomy, seeing bright red bleeding 3 weeks post-op is a major red flag. It's not hormonal; it's a surgical complication. You also need to distinguish between hormonal spotting and structural interference. Fibroids or polyps can mimic perimenopausal irregularity. They're physical obstacles that cause heavy bleeding regardless of your estrogen levels. When you visit your OB-GYN, bring your data. They don't just need to know you're bleeding. They need to know the frequency, the volume, and the associated symptoms like pelvic pain.
Diagnostic Tools and What to Ask For
A single blood test rarely captures the whole picture. Your FSH levels can swing wildly within 24 hours. One "normal" result doesn't mean you aren't in perimenopause. Ask for a transvaginal ultrasound to measure the thickness of your uterine lining. If the lining is abnormally thick, an endometrial biopsy might be necessary to rule out cellular changes. These tools provide the objective proof your symptoms deserve.
Most clinical guides ignore the data on your wrist. Your wearable devices track the physiological stress that often precedes a "flooding" episode. A sudden drop in Heart Rate Variability (HRV) combined with disrupted sleep can predict a heavy bleed before it starts. Don't just track the blood. Anticipate the disruption by integrating your wearable data with your symptom logs. This comprehensive view turns a confusing doctor's visit into a data-driven consultation. You're the expert on your body. We provide the evidence.
From Tracking to Anticipation: Taking Control with Solena
Most apps act like a rearview mirror. They record what happened yesterday. In midlife, a history of regular cycles doesn't help you plan next week's travel or a critical boardroom presentation. You need to move from passive tracking to active anticipation. Solena shifts the narrative from reaction to probability. It's about knowing the perimenopause bleeding patterns what to expect before they manifest physically. Tracking is history. Anticipation is power.
Our AI doesn't just look at a calendar. It analyzes high-fidelity data from your daily life. By monitoring sleep quality and basal temperature shifts, Solena identifies the subtle physiological markers of a hormonal surge or dip. Integrating wearables like the Oura Ring allows for effortless data collection. Your body speaks in data points like heart rate variability and core temperature. We translate those points into a 3-day window of foresight. You get an alert before the chaos starts. No more surprises. Just preparation.
Personalized Wellness Plans
Knowing a shift is coming is only half the battle. You need an actionable plan. Solena generates routines based on where your hormones are likely to be tomorrow. If the data suggests an estrogen spike, your plan might prioritize specific anti-inflammatory nutrition or adjusted exercise intensity to mitigate breast tenderness. If you aren't sure where you stand in this transition, start with the Am I in Perimenopause? Quiz. It's an immediate assessment designed for the 2026 health landscape. You can align your lifestyle with your biology in real time.
The Power of Probabilities
Traditional "period math" is exhausting and often incorrect during perimenopause. Solena replaces a fixed date with a likelihood percentage. Receiving a notification of a "70% chance of a heavy cycle" within the next 48 hours is more useful than a broken calendar prediction. It reduces the mental load. It allows you to pack what you need and clear your schedule. You aren't just monitoring a biological transition; you're managing it with sophisticated foresight. It's time to stop wondering and start knowing. Anticipate your symptoms with Solena and reclaim your schedule today.
Reclaim Your Schedule with Data
Unpredictable cycles don't have to dictate your life. Irregular flow is a biological reality of the 4 to 10 year perimenopausal transition. From the "Soaked Pad" rule to the mechanics of estrogen spikes, you now have the framework for perimenopause bleeding patterns what to expect. Knowledge is the first step. Data is the second.
Solena replaces the guesswork of traditional calendars with AI-powered hormonal anticipation. By syncing with your Oura Ring and Apple Health, we provide personalized wellness plans based on your unique physiological shifts. Stop looking back at what happened. Start preparing for what's next. You deserve a sophisticated partner that stays one step ahead of your biology. Reclaim your confidence with a system built for the modern woman.
Stop tracking and start anticipating your symptoms with the Solena App. Your transition is unique. Your support should be too. You're in control now.
Frequently Asked Questions
Is it normal to have two periods in one month during perimenopause?
Yes. Shortened cycles, or polymenorrhea, are a hallmark of the early transition. Your brain surges FSH to stimulate the ovaries, often causing ovulation to occur much earlier in the cycle. This can reduce a standard 28-day rhythm to 21 days or fewer. It's a common biological recalibration.
What does perimenopause spotting look like compared to a regular period?
Spotting is typically light, intermittent, and doesn't require a standard pad or tampon. It often appears as pink or brown streaks. A regular period involves a continuous, heavier flow that lasts several days. Spotting usually signals a temporary estrogen dip rather than a full lining shed.
Can I still get pregnant if my bleeding patterns are irregular?
Yes. You can still ovulate even when your cycles are unpredictable. Pregnancy remains a possibility until you have reached the 12-month milestone of no bleeding. Some women even experience "double ovulation" during this phase. Don't assume irregularity equals infertility.
How long do the irregular bleeding patterns of perimenopause typically last?
The entire perimenopause transition typically spans 4 to 10 years. Patterns often evolve during this window. You might start with shorter cycles and move toward skipping months entirely as you approach menopause. Understanding perimenopause bleeding patterns what to expect helps you navigate this decade with data-driven confidence.
Why is my perimenopause period blood suddenly bright red and watery?
Bright red blood indicates active, rapid shedding. The watery consistency often happens when estrogen levels are exceptionally high, creating a vascular but thin lining. This blood hasn't had time to oxidize or mix with significant cervical mucus. It's a sign of a fast-moving cycle.
What happens if I have heavy bleeding for more than 10 days?
Bleeding that lasts longer than 7 to 10 days consistently is a clinical red flag. It suggests your uterine lining is unstable, likely due to a lack of progesterone. This increases your risk for iron-deficiency anemia. If you're soaking a pad every hour, contact your doctor to rule out polyps or fibroids.
Can stress make my perimenopause bleeding patterns worse?
Yes. High cortisol levels act as a biological accelerant for cycle chaos. Cortisol and progesterone share the same molecular precursors. When you're stressed, your body prioritizes cortisol, which "steals" the building blocks needed to stabilize your uterine lining. Stress turns a shift into a disruption.
Is brown discharge for a week before my period a sign of perimenopause?
Brown discharge is simply oxidized blood that is shedding slowly. This "slow start" is a very common early indicator of perimenopause bleeding patterns what to expect. It happens when progesterone levels begin to falter. The lining starts to crumble slightly before the full hormonal signal to shed arrives.
Disclaimer
Solena is designed to support awareness, not replace care. It does not provide medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional for medical guidance.




